Ronald M. Burde Surgical Simulation Laboratory
 |
|
Resident physician David Poulsen (sitting) teaches microsurgical suturing skills to fellow resident Gabriel Rand. Medical students are frequently involved in the department’s research efforts, many of which utilize the advanced equipment available in the wetlab itself. |
 |
|
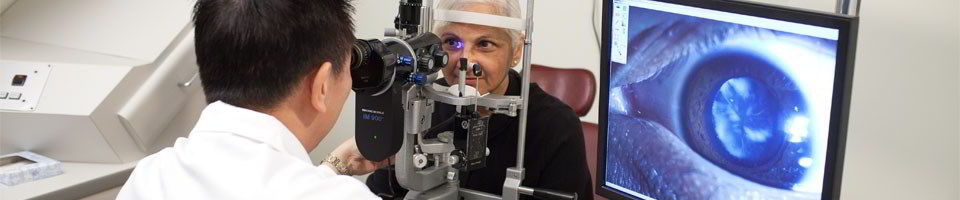
(Left to Right) Director of Refractive Surgery Jimmy K. Lee, MD and Department of Ophthalmology and Visual Sciences Chairman Roy S. Chuck, MD gather to share cataract surgery techniques with a resident at a Kitaro DryLab station. There are eleven Kitaro DryLab kits each with a dedicated set of instruments to practice with. |
The Ronald M. Burde, MD, Microsurgical Simulation Laboratory was established in 2013, and is housed within the Center for Ophthalmic Innovation (COIN), a collaboration that defines the Department’s dedication to combining surgical teaching with research and device development. The Center provides residents with access to one of the most advanced ophthalmic surgical training facilities in the country. The laboratory is available 24/7, and allows residents the ability to perform complex eye procedures, including entire cataract operations, in a highly realistic simulated environment. Phacoemulsification units are permanently housed in the laboratory to allow for training on multiple commonly used platforms. The Burde Laboratory is amongst the most advanced multimedia surgical training facilities in the world, and holds the distinction of being the featured wetlab in the American Academy of Ophthalmology’s EyeWiki article on the subject. A surgical wetlab curriculum has been incorporated and organized into the monthly academic calendar, and residents are trained by our subspecialty faculty in a variety of division-specific skill transfer sessions. A 3D virtual reality anatomy simulator is housed in the laboratory, allowing users to view and manipulate complex eye and brain structures, far beyond what is possible from a traditional anatomy atlas or textbook.
 |
|
Director of Retina, Umar Mian, MD (left) and resident physician Juliana Gildener-Leapman (right) inspect the ultrasound probe used in cataract surgery. In the foreground, one of the several phacoemulsification machines sits primed for a mock cataract surgery. |
Though all of the surgeries in the wetlab are for practice, all of the phacoemulsification machines are fully functional and operating-room ready. The wetlab boasts multiple phacoemulsification systems, many of which are the standard in many operating rooms today. Providing residents with modern and realistic practice tools translates to better preparation for the operating room and superior patient care.
The laboratory has a total of 14 (expanding to 20) video-enabled microscope stations featuring iPad integration, digital whiteboards, and a multimedia conference center housed within the facility that allows for a combined didactic experience.
The laboratory allows residents endless opportunities to improve their surgical skills well before operating on a live human eye. The facility continues to undergo expansion, serving as a community educational resource laboratory, innovation center and local training site for multiple national device manufacturers. The Burde Laboratory has helped define the Department of Ophthalmology’s commitment to resident education, training some of the best ophthalmic surgeons in the country.