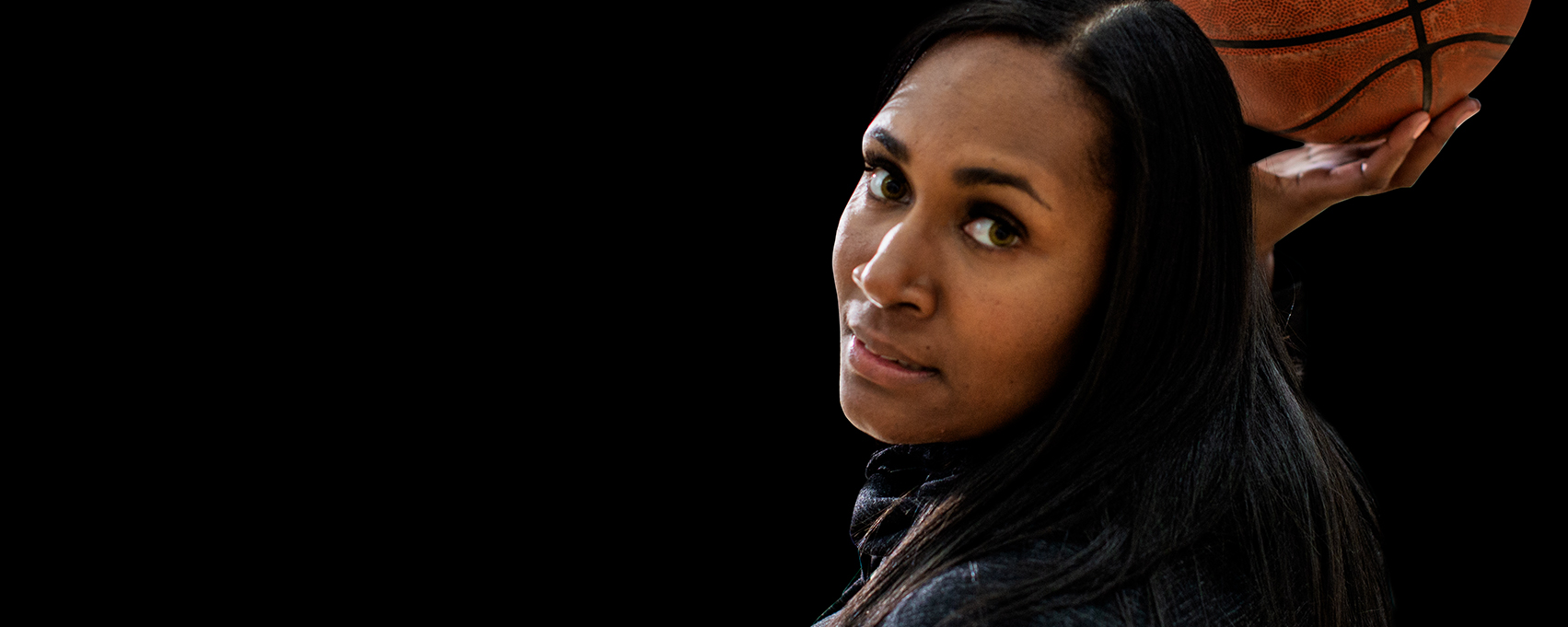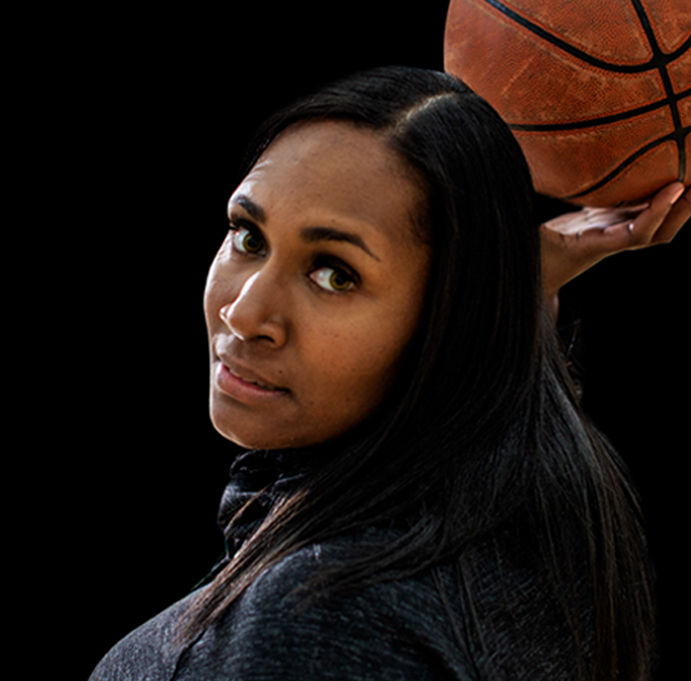Jessica
Jessica Green had been living with a damaged heart for as long as she can remember. At fifteen she was diagnosed with cardiomyopathy, and by twenty-one she had a pacemaker. But Jessica never let those things slow her down. She would run, play volleyball, and shoot hoops without issue. Until everything changed just before her twenty-ninth birthday.



Doctors at Montefiore discovered Jessica’s heart was pumping at just five percent of capacity.
“Her quality of life and her survival was measured in weeks to months at best.”

Jessica’s only chance of survival was immediate surgery to receive a left ventricular assist device (LVAD), an implanted mechanical pump designed to help her weakened heart circulate blood throughout her body.

The LVAD dramatically changed Jessica’s life. No longer weak and winded, she was able to resume most of the activities she loves. She even began volunteering at Montefiore, counseling patients going through the same cardiac issues she had dealt with.


Though Jessica’s health was vastly improved, her LVAD was just a temporary fix. The only permanent solution would be a heart transplant. But before she could be added to the national transplant list, she would have to lose some weight.

“We know that morbid obesity is a problem for transplant patients. So all transplant programs have a limit, a cut-off on what we call BMI, body mass index. Above that cut-off we don’t offer transplants. So Montefiore has a team of nutritionists and exercise physiologists that can help patients lose the weight. And if that doesn’t work, we can also offer patients bariatric surgery designed to reduce the size of the stomach in order to lose weight. At Montefiore, we have the largest bariatric surgery program in the country, having done over 1,300 last year.”

Within months, Jessica lost over 100 pounds and had her name added to the national heart transplant list. And then, after four long years of waiting, Jessica finally received the fully functioning heart she had always dreamed of.

“I’m so lucky to get a second chance. I’m so thankful. I’m so happy. Thank you, Montefiore.”
Meet Dr. Daniel Goldstein
Professor, Cardiothoracic and Vascular SurgeryVice Chairman, Cardiothoracic and Vascular Surgery,
Director, Mechanical Assistance Program
Co-Director, Center for Advanced Cardiac Therapy
Surgical Director of Cardiac Transplantation