Heart Transplant Three Year Survival Rate:
Comparison to National Data*
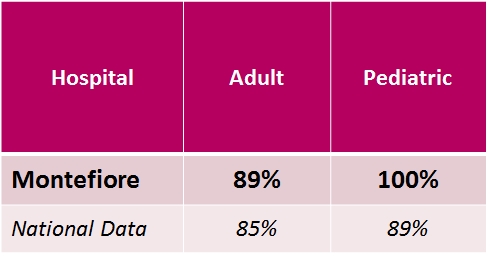
*January 2018 Scientific Registry of Transplant Recipients
(SRTR) Report
During heart transplantation a patient's diseased heart is replaced with a healthy donor heart. In the United States, there are between 60,000 and 100,000 people who could benefit from a new heart. But due to an acutely limited supply, only 2,300 to 2,400 transplants are performed each year. Because of the large discrepancy between demand and supply, heart transplants are reserved for patients with severe end-stage heart disease.
The procedure for a heart transplant begins with an evaluation by a multidisciplinary medical team. This team examines four main points:
Is the Patient Medically Fit?
Is the patient sick enough to need a new heart? If so, are there any other medical conditions that would render the patient ineligible for transplant? For example, a patient with kidney failure is not eligible for transplant.
Does the Patient have the Necessary Social Support?
Heart transplant is not a procedure patients can go through alone. Patients should have strong social support.
Is the Patient Psychologically Fit?
Transplant patients must adhere to strict behavior modifications and regimented rejection medication. Patients should demonstrate an ability to remain compliant long term.

*January 2018 Scientific Registry of Transplant Recipients
(SRTR) Report
The Department of Cardiovascular and Thoracic Surgery is renowned for being at the forefront of cutting edge therapies. The recruitment of Patients on the transplant list are assigned priorities based on the severity of their conditions. The highest priority is given to patients in rapid decline, generally patients on intravenous medications, balloon pumps and/or VADs. Lowest priority is assigned to patients with stabilized heart failure. Often these patients are at home.
Once priority is established, other factors help determine who gets an available donor heart, including:
Geography
Once harvested, a heart must be transplanted within four hours, to remain viable. For example, Montefiore Einstein Center for Heart and Vascular Care patients cannot safely receive hearts from donors in Los Angeles, but they could receive hearts from Boston.
Blood Type
Donors and recipients must have compatible blood types.
Body Size
Donors and recipients must have compatible body sizes. For example, a heart from a six-foot donor may be too large for a five-foot recipient.
Waiting Time
When two recipients are equally compatible matches, the heart goes to the patient who's been waiting longer and is sicker.
Transplant Procedure
To make sure that no more than four hours pass between harvesting the heart and transplant, the surgical team who removes the heart from the donor is in constant contact with the recipient team at the Heart Center.
While waiting for the heart to arrive, the recipient is prepared for surgery as quickly as possible. The patient is placed on a heart-lung machine, and upon arrival of the donor heart, the surgeons remove the recipient's diseased heart, then prepare and implant the new heart.
Following the 90-minute procedure, the patient is removed from the heart-lung machine. Once the heart function is stable, the patient is moved to the intensive care unit for further care.
Risk of Rejection
Rejection occurs when the patient's immune system recognizes the new heart as foreign and mounts an immune reaction to it. The new heart is biopsied routinely to look for evidence of rejection; if necessary, immunosuppressive medication is adjusted.
At home, patients watch for other signs of rejection, including shortness of breath, flu-like symptoms, and low-grade fever. Although patients must take anti-rejection medication for the rest of their lives, the first year following transplant is the most critical. Fortunately, severe rejection is very rare. Most cases can be handled with by increasing rejection medications.