Diagnostic and Therapeutic Procedures
Using advanced techniques and state-of-the-art technology, our team of world-renowned cardiac electrophysiologists offers early detection of and treatment for a vast spectrum of conditions relating to cardiac arrhythmia. The procedures listed below are a selection of options available to our patients.
-
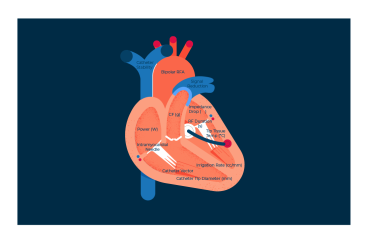
This definitive approach eliminates tissue that causes arrhythmias in the majority of patients. The most common procedures we perform are:
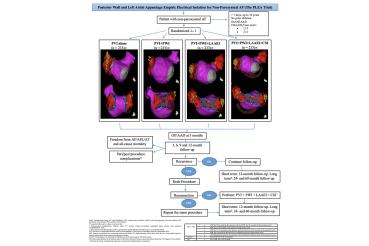
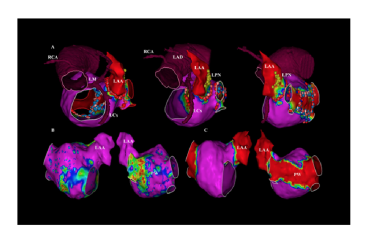
● Atrial Fibrillation (Radiofrequency and Cryo Energy)
● Atrial Flutter
● Ventricular Tachycardia (Endocardial & Epicardial Mapping/Ablation)
● Ventricular Fibrillation
● Supraventricular Tachycardia (SVT)
● Premature Ventricular Contractions (PVC) -
The left atrial appendage is a structure in one of the upper chambers of the heart on the left side, in which clots are formed during atrial fibrillation. These devices reduce the risk of stroke in patients with this arrhythmia who have a high risk of bleeding, falls, or poor compliance to blood thinners. The most studied devices we implant are the WATCHMAN™ device, the Amplatzer™ Cardiac Plug, and the LARIAT® Suture Delivery Device. Our institution is considering implanting newer devices currently under investigation, such as the Coherex® WaveCrest System.
WATCHMAN™ Device
LARIAT® Suture Delivery Device
-
Cardiac Resynchronization Therapy (CRT) involves the placement of an implantable biventricular pacing device that synchronizes contractions. This device enhances the pumping efficiency of the heart, which can be associated with an increased capacity for exercise, reduced hospitalization time, and significantly lower mortality rates. His bundle pacing (HBP), one of the newest treatments available, has been shown to improve outcomes by promoting a more physiologic or “natural” stimulation.
-
In some cases, we implant small devices (pacemakers) underneath the skin which help monitor the heartbeat and send out an electrical impulse when slowed beyond an acceptable level. Two of the newest pacemaker options we offer are:
● His bundle pacing (HBP), one of the newest treatments available, has been shown to improve outcomes by promoting a more physiologic or “natural” stimulation
● Leadless pacemakers are wireless and can reduce the risk of associated infections
Leadless Pacemaker
-
These devices send an electric shock to revert serious ventricular arrhythmias, such as tachycardia and fibrillation, back to a normal heartbeat, significantly minimizing the risk of sudden cardiac arrest.
Subcutaneous ICD
-
A special team evaluates the pacemakers and implantable cardioverter defibrillators (ICDs) of Arrhythmia Center patients. Removal of the pacemaker or implantable cardioverter defibrillators (ICD) wires might be necessary in cases where these are damaged, infected, or causing blockage. Using laser sheaths to remove the damaged wires increases success rates and significantly minimizes complications.
-
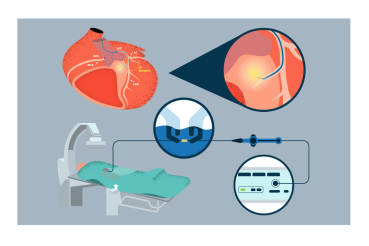
This test studies the electrical conduction of the heart to determine why its beats may be irregular. During this study, catheters are placed inside the heart to find out where the arrhythmia is coming from and how it should be treated. Electrophysiology testing can also be used to evaluate the risk of arrhythmia formation in certain heart conditions.
-
This program performs cardiac sympathetic denervations to treat refractory ventricular arrhythmias in patients with ischemic and non-ischemic cardiomyopathies. It can also be used in patients with inherited primary arrhythmia disorders, such as long QT syndrome and catecholaminergic polymorphic ventricular tachycardia (CPVT), with the goal of helping to eliminate living with implantable cardioverter defibrillators (ICD) shocks.
-
This device is implanted to assess atrial fibrillation and monitor for arrhythmias in patients with cryptogenic stroke. It measures and records their heartbeat over time as they go about their daily activities.
-
Fluoroless procedures use minimal to no radiation, thereby preventing unnecessary exposure.
-
In certain cases, this procedure is used to restore normal heart rhythm before or instead of ablation.
-
Tilt table testing helps doctors identify the cause of fainting by evaluating how changes in body position can affect blood pressure and heart rate.